What Does a Comprehensive Spinal Evaluation Include?
April 24, 2026
10 min

Why a Thorough Spinal Evaluation Matters
An accurate spinal assessment begins with a detailed patient history that captures symptom onset, lifestyle, past injuries and systemic factors. The clinician then proceeds through systematic inspection, palpation, range‑of‑motion testing, neurological screening and special orthopedic maneuvers—steps outlined in evidence‑based guides from orthopaedics and chiropractic curricula. By integrating posture analysis, gait observation, functional movement screening and, when needed, imaging or laboratory studies, the examiner creates a full picture of structural, muscular and neural contributors. This holistic, patient‑centered approach respects each individual’s unique biomechanics, stressors and wellness goals, allowing the practitioner to tailor spinal adjustments, therapeutic exercises, ergonomic advice and stress‑reduction techniques such as yoga or meditation. When the evaluation informs a personalized plan, it not only relieves current pain but also identifies preventive strategies that protect spinal alignment, improve function and support long‑term health. Regular follow‑up visits monitor progress, refine interventions, and reinforce healthy habits, ensuring sustained spinal resilience and overall vitality.
History Taking, Red‑Flag Screening, and the Most Common Spinal Disorder
 A comprehensive spinal evaluation begins with a detailed patient history that records the exact location of pain, radiation patterns, onset (sudden or gradual), duration, aggravating and relieving factors, prior injuries, surgeries, medications, and lifestyle influences such as work ergonomics and exercise habits. Early functional questions probe how pain limits walking, lifting, sitting, sleeping and daily tasks, and may include a brief disability questionnaire (e.g., Oswestry).
What is the most common spinal disorder? Low back pain is the most prevalent spinal condition, affecting up to 80 % of adults in the U.S. It often stems from musculoskeletal strain, degenerative disc changes, or inflammatory arthritis and is a leading cause of work disability.
Back pain assessment questions – The clinician asks where the pain is, whether it radiates, its intensity on a 0‑10 scale, onset timing, triggers (movement, posture, rest), and functional impact. Red‑flag symptoms—such as age > 50, unexplained weight loss, fever, night‑time pain that awakens the patient, progressive neurologic deficits, recent trauma, and localized spinal tenderness suggesting infection, tumor, or fracture. Presence of any red‑flag symptoms warrants immediate imaging and specialist referral.
Systematic Inspection and Postural Analysis

The exam starts with hand hygiene, patient ID and consent, then the patient stands barefoot.
General inspection (look) includes anterior, lateral, and posterior views: note habitus, skin changes, scars, assistive devices; assess cervical lordosis, thoracic kyphosis (20‑45°) and lumbar lordosis, and check for scoliosis, pelvic tilt or muscle wasting.
Gait assessment follows—observe stride length, antalgic limp, foot‑wear wear and any Trendelenburg or waddling patterns.
Curvature evaluation proceeds with active and passive ROM: cervical flexion/extension (0‑80°/0‑50°), thoracic rotation, lumbar flexion/extension and lateral flexion, noting restrictions or pain.
Spine examination checklist: After hygiene and consent, expose the patient and perform inspection of posture, gait and spinal curves from angles.
Palpate spinous processes, sacroiliac joints and paraspinal muscles for tenderness or step.
Test ROM (flexion, extension, lateral flexion, rotation) for cervical, thoracic and lumbar regions.
Conclude with a neurologic screen (reflexes, sensation, strength and special tests such as Straight Leg Raise, femoral nerve stretch and Schober’s test, then summarize findings and next steps.
Palpation, Manual Assessment, and Early Signs of Segmental Dysfunction
 A thorough lumbar spine exam starts with static palpation of the spinous processes, vertebral bodies, and adjacent paraspinal muscles to locate tenderness, muscle spasm, and step‑offs that suggest facet or joint restriction. Motion palpation—either seated or supine—allows the clinician to feel vertebral glide and identify hypomobility or hyper‑mobility segments. Early clinical clues for nerve‑root compression include localized pain with specific movements, altered sensation in the corresponding dermatome, and subtle weakness in the related myotome.
What are the components of a lumbar spine examination?
The exam begins with inspection of posture, alignment, and skin changes, followed by static and motion palpation to detect tenderness or step‑offs. Active and passive range‑of‑motion testing evaluates flexion, extension, lateral bending, and rotation. Neurologic assessment checks deep‑tendon reflexes, dermatomal sensation, and muscle strength. Finally, orthopedic maneuvers such as straight‑leg raise, slump test, and facet‑compression test help pinpoint structural sources of pain.
What are the first signs of L4‑L5 compression?
Early signs often start with dull lower‑back ache that worsens with sitting or forward bending. L4 involvement may radiate pain to the inner thigh and knee, with numbness in the medial lower leg and weakened quadriceps. L5 compression typically produces pain down the lateral thigh to the top of the foot, tingling in the first webspace, and diminished foot dorsiflexion. A reduced patellar reflex may also signal L4 irritation.
Active Range‑of‑Motion and Special Orthopedic Tests
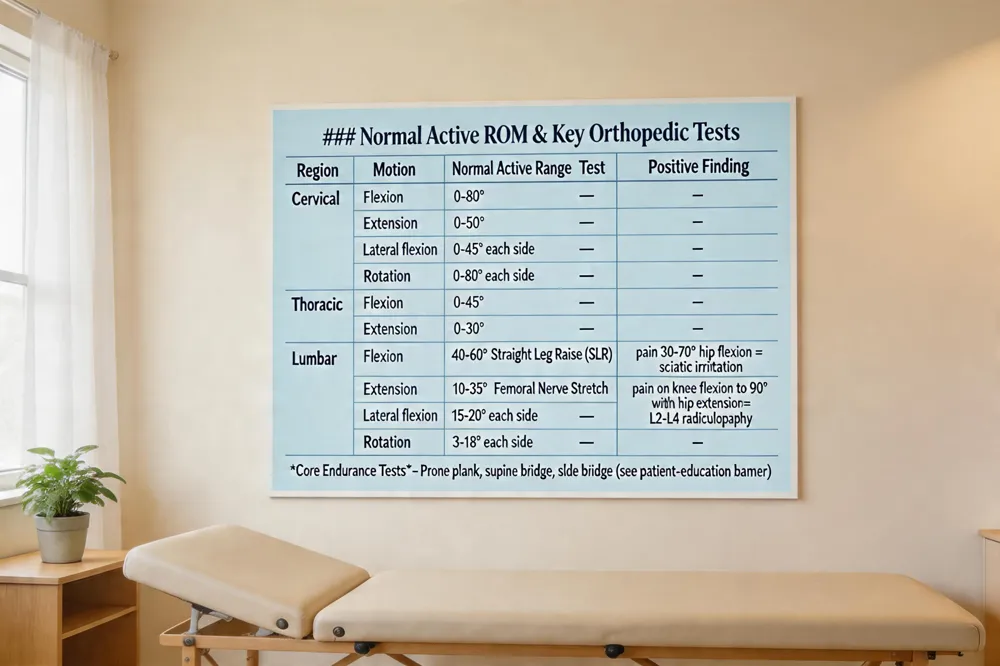 A complete spinal assessment starts with measuring normal motion ranges: cervical flexion 0‑80°, extension 0‑50°, lateral flexion 0‑45°, rotation 0‑80°; thoracic flexion 0‑45°, extension 0‑30°; lumbar flexion 40‑60°, extension 10‑35°, lateral flexion 15‑20° each side, rotation 3‑18° each side. Special tests that follow include the modified Schober’s test (≥5 cm increase, >20 cm total) for lumbar flexion, the Straight Leg Raise (pain between 30‑70° hip flexion indicating sciatic irritation) and the femoral nerve stretch test (pain on knee flexion to 90° with hip extension) for upper lumbar radiculopathy. Core stability for low‑back health is evaluated with three functional tests: the prone plank bridge, supine bridge, and side (lateral) bridge, which assess endurance of the deep stabilizers.
What are three special tests to perform on the low back? The most frequently used functional tests are the prone plank bridge, supine bridge, and side bridge (lateral plank). These assess core endurance and stability in patients with low‑back complaints.
What are the components of a lumbar spine examination? It begins with visual inspection of posture, alignment, and skin changes, followed by palpation of spinous processes and paraspinal muscles for tenderness or step‑offs. Next, ROM testing (flexion, extension, lateral bending, rotation) is performed, then neurologic assessment (reflexes, sensation, muscle strength). Finally, orthopedic maneuvers such as Straight Leg Raise, slump test, and facet‑compression test are used to localize pain sources.
Neurologic Screening and the Back‑Pain Diagnostic Chart
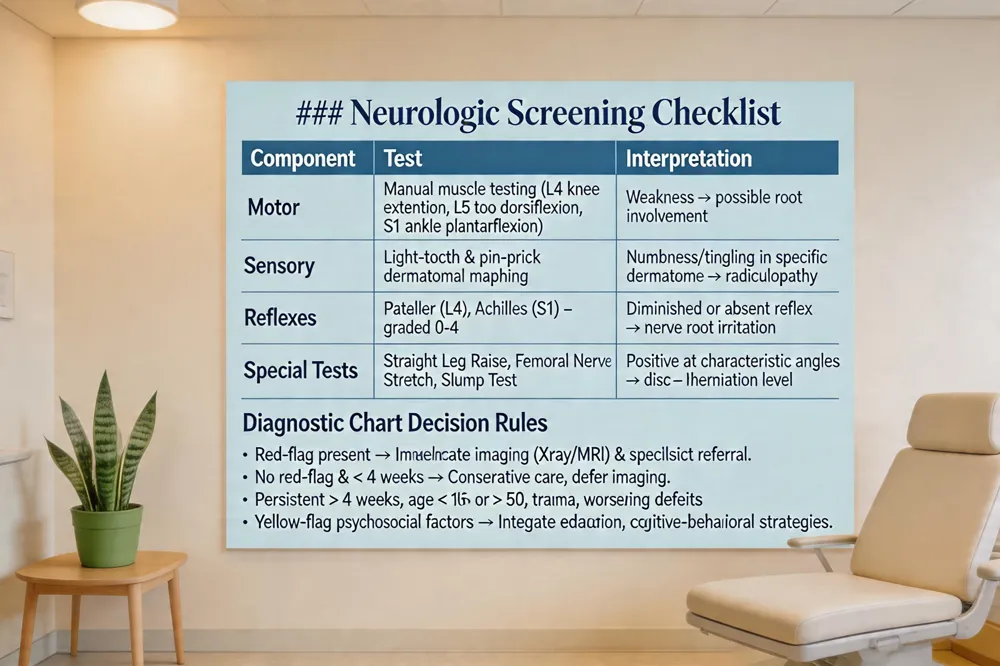 A thorough neurologic screen is the cornerstone of any back‑pain diagnostic chart. Clinicians evaluate motor function by manual muscle testing of key myotomes (e.g., L4 knee extension, L5 toe dorsiflexion, S1 ankle plantarflexion). Sensory assessment maps dermatomal light‑touch and pin‑prick perception, while deep‑tendon reflexes—patellar (L4) and Achilles (S1)—are graded to detect nerve‑root irritation.
The chart uses these findings to decide when imaging is warranted: if red‑flag signs (unexplained weight loss, fever, night pain, bowel/bladder dysfunction, or saddle anesthesia) are present, immediate X‑ray or MRI is ordered. In their absence, a normal neurologic exam and a symptom duration under four weeks typically defer imaging, reserving it for persistent pain, age <16 or >50, significant trauma, or worsening deficits.
Red‑flag results flag yellow‑flag psychosocial factors (fear‑avoidance, depression) are integrated into the chart to guide patient‑centered treatment—combining chiropractic adjustments, therapeutic exercise, ergonomics, and education—while scheduling follow‑up reassessments to monitor progress and prevent chronicity.
Imaging, Laboratory Tests, and Adjunctive Therapies
 A thorough spinal assessment uses imaging only when red‑flag signs or persistent neurologic deficits are present. X‑rays are ordered for suspected fractures, spondylolisthesis or alignment abnormalities; MRI is the modality of choice for disc herniation, nerve‑root compression, infection, or inflammatory disease; CT provides high‑resolution bone detail when MRI is contraindicated or for surgical planning. Laboratory studies (CBC, ESR, CRP, metabolic panels) are reserved for ruling out systemic infection, inflammatory arthritis, or metabolic bone disorders that may mimic spinal pathology.
Adjunctive therapies such as magnesium supplementation can support muscle relaxation and reduce spasm associated with spinal stenosis, offering modest pain relief and improved mobility. Magnesium does not reverse canal narrowing, so it should be integrated with chiropractic adjustments, core‑strengthening exercises, low‑impact exercise, weight management, and patient education. Always discuss supplement use with your chiropractor or healthcare provider before adding it to your regimen.
Personalized Treatment Planning and the Biochemical Impact of Adjustments
 Spinal adjustments, therapeutic exercise, and lifestyle counseling are pillars of a patient‑centered plan. After a thorough history and inspection, the chiropractor applies low‑force or high‑velocity adjustments to restore joint mobility. Research shows a short course of adjustments lowers circulating pro‑inflammatory mediators such as IL‑6, TNF‑α, CRP and prostaglandins, indicating the body releases “toxins” that are actually cytokines. The nervous‑system response also boosts endorphins and serotonin, supporting natural pain relief. Evidence‑based guidelines list spinal manipulation as an effective non‑pharmacologic option for acute low‑back and neck pain, with systematic reviews confirming modest pain reduction and functional gain. Side effects are usually mild—temporary soreness, stiffness, fatigue, or brief dizziness—while serious adverse events are rare when proper screening is performed. Disadvantages include multiple visits, variable insurance coverage, and a small risk of serious complications in high‑velocity neck techniques. Chiropractic care can also lower chronic cortisol by reducing sympathetic over‑activity, contributing to overall wellness.
Functional Outcome Measures, Maintenance Care, and Magnesium Support
 Patient‑reported disability indices such as the Oswestry Disability Index and Roland‑Morris Questionnaire give a quantitative picture of how low‑back pain limits daily activities. Tracking these scores over time allows the chiropractor to gauge the effectiveness of adjustments, therapeutic exercises, and lifestyle changes, and to modify the care plan when progress stalls.
Maintenance care focuses on regular spinal adjustments combined with ergonomic counseling—optimizing workstation setup, promoting neutral posture, and incorporating core‑strengthening routines. These strategies help preserve alignment, reduce recurrent strain, and support long‑term wellness without reliance on medication or surgery.
Magnesium can be a useful adjunct. It helps relax tight paraspinal muscles and diminish spasm‑related pain, which can improve mobility in conditions such as spinal stenosis. Magnesium does not reverse the anatomic narrowing of the canal, but when paired with gentle stretching, low‑impact exercise (walking, swimming, yoga), weight management, and targeted physical therapy, it can enhance overall comfort and functional outcome. Patients should discuss dosage and potential interactions with their chiropractor before adding magnesium to their regimen.
Patient Education, Core‑Strengthening, and Preventive Strategies
 A well‑rounded spinal health program starts with patient education. During the initial back‑pain assessment the clinician asks where the pain is located, whether it radiates, its onset, duration, intensity (0‑10 scale) and factors that improve or worsen it. Functional limitations, prior injuries, surgeries, and red‑flag symptoms such as unexplained weight loss, fever, night pain, or numbness are also explored, and standardized disability questionnaires (Oswestry or Quebec Back Pain Disability Scale) may be used to quantify impact.
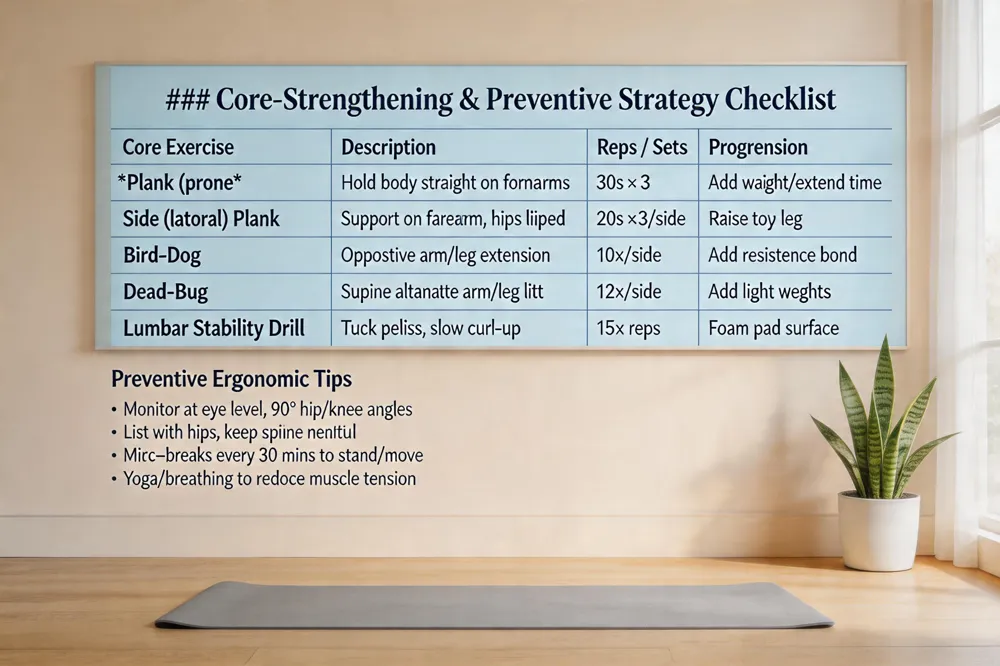
Core‑strengthening exercises—planks, bird‑dogs, dead‑bugs, and lumbar stability drills—reinforce deep abdominal and multifidus muscles, supporting proper posture and reducing spinal load. Posture correction drills, including mindful sitting with lumbar support and shoulder retraction, are taught and reinforced during visits.
Ergonomic adjustments for workstations (monitor at eye level, chair height allowing 90° hip/knee angles) and daily activities (lifting with hips, avoiding prolonged static positions) prevent repetitive strain.
Stress‑reduction techniques such as yoga, meditation, and controlled breathing relax paraspinal muscles, lower sympathetic tone, and complement chiropractic care by minimizing muscle tension that can exacerbate misalignments.
Putting It All Together for Long‑Term Spinal Wellness
A comprehensive spinal evaluation at Back in Action Bodyworks begins with a thorough health history that captures symptom onset, lifestyle factors, and past medical treatments. The physical exam follows a systematic four‑step approach—inspection of posture and gait, palpation of spinous processes and paraspinal muscles, active and passive range‑of‑motion testing, and a full neurological screen (motor strength, sensory mapping, reflexes). Special orthopedic tests such as the straight‑leg raise, Schober’s test, and Kemp test help pinpoint disc, facet, or nerve involvement, while functional movement analysis reveals how spinal health influences daily activities. Follow‑up visits are scheduled regularly to monitor progress, reassess red‑flag signs, and adjust the treatment plan based on objective outcome measures like the Oswestry Disability Index. Throughout, Back in Action Bodyworks remains committed to evidence‑based, holistic care—integrating chiropractic adjustments, therapeutic exercise, ergonomic counseling, and stress‑reduction techniques to promote lasting spinal alignment and overall wellness.
Recent articles

What Does a Comprehensive Spinal Evaluation Include?

Success Spotlight: Transformative Results After Six Weeks of Chiropractic Treatment

Understanding the Initial Assessment Process in Chiropractic Care

Designing a Personalized Corrective Exercise Plan for Chronic Pain Management
Natural Pain Management: Combining Acupuncture, Yoga, and Chiropractic
Chiropractic Care vs. Pain Meds: Long-Term Outcomes for Back Pain Sufferers

What to Expect During a Sciatica‑Focused Decompression Session

Understanding the Pain-Relief Mechanics Behind Chiropractic Adjustments
Success Rates of Non‑Surgical Spinal Decompression for Sciatica

Patient-Centered Chiropractic Care: Personalized Plans for Back Pain Relief
How Chiropractic Treatments Reduce Inflammation and Speed Up Back Pain Recovery
Real‑Life Stories: How Chiropractic Helped Patients Overcome Chronic Back Pain

From Symptom Masking to Root‑Cause Healing: A Practical Guide

6 Holistic Non‑Surgical Treatments That Deliver Sustainable Back‑Pain Relief
Key Questions to Ask When Selecting Your Chiropractor

Mindful Movement: Incorporating Stretch Breaks Into a Busy Day

Why Targeting the Underlying Cause Beats Temporary Symptom Relief
8 Ways Physiotherapy Complements Chiropractic Adjustments for Faster Recovery

Meal Planning for Athletes Recovering from Back Injuries

9 Everyday Lifestyle Tweaks to Preserve a Healthy Spine and Prevent Pain

Functional Movement Screening for Root‑Cause Pain Identification

6 Things You’ll Experience During Your First Chiropractic Appointment

Spinal Decompression vs. Standard Physical Therapy for Sciatica: A Comparative Review

New Findings on How Adjustments Influence Blood Circulation

Work‑From‑Home Ergonomics: A Blueprint for a Pain‑Free Back

The Link Between Chiropractic Care and Improved Sleep Quality

Physiotherapy Techniques That Strengthen the Benefits of Chiropractic Adjustments

Biomechanical Insights Behind Successful Spinal Decompression

Desk‑to‑Dumbbell: Lifestyle Shifts That Guard Your Lower Back

10 Corrective Exercises for Sustainable Pain-Free Living

Morning Routines That Support Spine Health and Reduce Stiffness
Calcium and Magnesium‑Focused Nutrition for Bone Density and Spine Health

9 Ways Chiropractic Care Transforms Back Pain Management

Testimonial: Nutrition‑Guided Recovery Accelerated by Chiropractic
Science‑Backed Spinal Decompression for Relieving Sciatica Symptoms

Key Questions to Ask During Your Initial Chiropractic Consultation
Whole‑Body Wellness Blueprint: Nutrition, Exercise, and Chiropractic Synergy

A 12‑Week Corrective Exercise Blueprint for Chronic Neck Discomfort

Manual Therapy Plus Targeted Exercise: Accelerating Post‑Injury Recovery

Home‑Based Spinal Decompression Devices: What Patients Should Know

Chiropractic Care Statistics: Reducing Lost Workdays From Back Pain

How Targeted Nutrition Enhances Immune Function and Lowers Inflammatory Pain
Self‑Assessment Tools to Identify Hidden Triggers of Back Pain

Preparing for Your First Chiropractic Appointment: A Practical Checklist

Back Pain Relief Benefits: Lower Opioid Use and Better Quality of Life

Foam‑Rolling Techniques to Complement Chiropractic Adjustments
Progressive Overload Principles in Corrective Exercise Programs

Six‑Month Transformation: Integrated Care Success Story

7 Nutritional Hacks to Boost Your Overall Wellness
How to Choose a Chiropractor: Credentials, Techniques, and Patient Compatibility
5 Ways Spinal Decompression Can Ease Sciatica Pain

Overcoming Sciatica: A Patient’s Multidisciplinary Treatment Journey
Lifestyle Changes That Promote a Healthy Spine

Physiotherapy as a Complement to Chiropractic Treatments

6 Ways Physiotherapy Enhances Chiropractic Treatment Outcomes

Daily Living Tips for a Strong and Healthy Spine

How Physiotherapy Enhances Chiropractic Outcomes
Holistic Treatments: Alternatives to Surgery for Pain Relief
Inspiring Patient Success Stories from Chiropractic Clinics
Integrating Physiotherapy with Chiropractic Treatments
Corrective Exercise Routines for Chronic Pain Prevention

10 Corrective Exercises to Maintain a Healthy Spine and Relieve Pain
Exercise Strategies for Long-Term Pain Management
The Importance of Treating the Root Cause of Pain
Nutritional Support Strategies for Whole-Body Wellness
7 Essential Questions to Ask When Choosing Your Chiropractor
Identifying and Addressing Root Causes of Pain
Maintaining a Healthy Spine with Lifestyle Adjustments
Sciatica Symptom Relief via Spinal Decompression
8 Reasons Why Addressing the Root Cause of Pain Is Crucial
Chiropractic Care’s Impact on Back Pain Recovery
Combining Physiotherapy with Chiropractic Care for Better Results

Inspiring Recovery: Chiropractic Patient Testimonials
Nutritional Counseling Tips for Optimal Wellness

Why Addressing the Root Cause of Pain is Crucial
Back Pain and Chiropractic Care: A Winning Combination
Chiropractic Care Benefits You Might Not Know
Exploring Holistic and Non-Surgical Treatments for Pain
Spinal Health: Lifestyle Tips for Everyday Wellness
Spinal Decompression Therapy: Benefits and Applications
Holistic and Non-Invasive Spine Care Options
Everyday Lifestyle Advice to Keep Your Spine Healthy
The Significance of Treating Root Causes in Pain Therapy
Best Corrective Exercises for Sustainable Pain Management
Addressing Underlying Causes of Pain for Long-Term Relief
6 Key Benefits of Spinal Decompression Therapy for Sciatica Relief
How Nutritional Counseling Supports Spine Health and Recovery

The Role of Physiotherapy in Supporting Chiropractic Treatments
What Happens During Your First Visit to a Chiropractor?
Holistic and Non-Invasive Treatments: Alternatives to Back Surgery
How Spinal Decompression Therapy Relieves Sciatic Nerve Pain
Real Patient Testimonials: Success Stories from Chiropractic Care
Understanding Spinal Decompression for Effective Sciatica Relief
What to Expect When Visiting a Chiropractor for the First Time
Benefits of Regular Chiropractic Adjustments for Back Pain Management
Patient Testimonials Highlighting the Benefits of Chiropractic Care

Corrective Exercise Routines Designed for Lasting Back Pain Relief
Lifestyle Recommendations for Sustaining a Healthy Spine
Nutritional Guidance to Support Spinal Function and Healing